Perspectives
Small populations, big dollars. Part 3
Hereditary Angioedema: Let’s not make health care itself a trigger
June 13, 2018Hereditary Angioedema. Some specialty conditions are rare, challenging to treat and difficult to live with. And the annual drug therapy price tag for members for these conditions can top $1 million. With stakes this high, specialty drug management becomes even more important. Read about three of them here.
Part 1: Hemophilia. Part 2: Myasthenia gravis. Part 3: Hereditary Angioedema.
Sometimes stress can aggravate a condition; and sometimes the health care system is a stressor.
People with rare conditions like hereditary angioedema (HAE) often have a challenging time with our complex health care system. Diagnosis can take an average of nine years. Until the member sees an article, or reads something online, they might endure years of misdiagnoses, useless prescriptions, and sometimes even unneeded, exploratory surgeries.1
Once diagnosed, a handful of drugs treat HAE, and those drugs have been around only about 10 years. The condition has three unique types, so a treatment regimen needs to be tailored to the type. Layer on challenges of navigating paperwork when your treatment runs into the hundreds of thousands of dollars. Sounds like a recipe for stress to me.
HAE causes painful swelling
This rare and potentially life-threatening genetic condition only occurs in about 1 in 50,000 people. It causes attacks of painful swelling in specific parts of the body including the stomach, hands, feet, arms, legs, throat, and face. Patients who suffer swelling in the intestinal wall often suffer excruciating abdominal pain, nausea and vomiting. Swelling of the airway or throat is particularly dangerous, because it can cause death by asphyxiation.2
Attacks can be caused by stress, fatigue, physical activity, dental work, illness, hormonal changes, medication, diet and more.
Drugs comprise 97 percent of the cost of care
Prime presented a study on HAE at the Academy of Managed Care Pharmacy’s (AMCP) Managed Care and Specialty Pharmacy conference in Boston this past April.
This study showed an average 12-month HAE total cost of care of $409,925, with HAE drug costs totaling $395,507 (97 percent). All other medical and pharmacy costs were just $14,418 (3 percent).
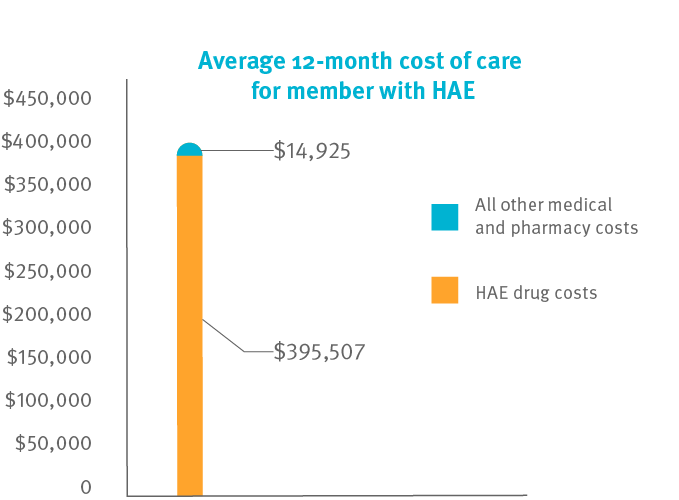
Some HAE drugs are for attacks, other HAE drugs are prophylaxis (preventive). Preventive treatment works for some, helping to stretch the time between attacks.
For the study, Prime analyzed 15 million commercially insured members pharmacy and medical claims . They found 226 members with an HAE drug claim. Of these, 111 (49 percent) met continuous enrollment criteria. Note these two interesting pieces of data:
- Ten of the 111 (9 percent) had more than $1 million in HAE drug spend. This accounted for 30 percent of the $43.9 million overall HAE drug spend in Prime’s commercial book of business.
- 40 percent of the original 226 were new starts to HAE drug therapy.3
Improving the quality of care for members with HAE
Here are three ways we can improve the quality of care for members with HAE:
Support for outliers. The ten members who are using more than $1 million in HAE drugs may need more help from the health care system than they are getting. They’ve been with the health plan awhile. Their use of drugs that treat HAE are outside the norm, as are charges for emergency room visits, hospital stays and other health care services. It may have built up slowly. Finding ways these members could cut costs while maintaining a high level of care is not going to be an easy fix, but it can be done.
In fact, check out this case study from Blue Cross & Blue Shield of Rhode Island. They have a great program of embedded pharmacists in medical clinics that allows for personalized attention for patients right in doctors’ offices. A pharmacist there worked with a woman with HAE for more than two years, attending doctor appointments, working with her through medication changes and helping her figure out lifestyle adjustments. Her drug costs went from $1.7 million a year to $975,000 a year.4
Monitoring new starts (members taking a drug for HAE for the first time). The 40 percent of new starts suggests there is some churn in this group. Maybe these members left a plan and came back. Maybe they went to another plan. A person with HAE may have difficulty with steady employment because of absenteeism caused by the condition. These new starts might reflect that. So, they may or they may not be newly diagnosed.
Ongoing pharmacist outreach from the very first fill. We believe this is how you can best support a member with HAE (and keep their costs from escalating outside the norms).
We know that most people with HAE have had a tough road getting to an accurate diagnosis. Once they have the HAE diagnosis, there are things we can do to help. A pharmacist case manager can be an advocate for a person with HAE, a bridge over the cracks in the health care system for patients with rare chronic diseases. A pharmacist can provide a focal point for the questions and challenges a newly diagnosed member with HAE will face the first months of treatment adjustments.
Prime projects that a program with six pharmacists providing case management to 52 members with HAE could help avoid $21 million in drug costs, for a possible 13:1 return on investment within one plan year.
Rare, but not insignificant
The numbers of members affected by rare conditions like HAE may be small, but the impact on people living with HAE can be huge. And the relative cost of care is too. All the stakeholders involved must work together to improve the quality of care and help control costs.
Drug names are the property of their respective owners.
References
- “Hereditary angioedema with C1 inhibitor deficiency: delay in diagnosis in Europe.” Zanichelli et al. Allergy, Asthma & Clinical Immunology 2013, 9:29. Accessed at: http://www.aacijournal.com/content/9/1/29
- “What is hereditary angioedema (HAE)?” ©2018 CSL Behring LLC. BRN15-09-0036(1). Accessed at: http://www.allabouthae.com/what-is-hae
Vande Walle SE, Starner CL, Gleason, PP. Hereditary Angioedema: A Comprehensive Integrated Medical and Pharmacy Claims Analysis of Utilization and - Costs among 15 Million Commercial Insured Members. Poster Presentation at AMCP meeting; April 2018 in Boston MA. Accessed at: https://www.primetherapeutics.com/content/dam/corporate/Documents/Newsroom/Pressreleases/2018/document-amcpspring18-hae.pdf
- Complete pharmacist integration delivers results. Blue Cross & Blue Shield of Rhode Island case study. April 27, 2018. Accessed at: https://www.primetherapeutics.com/en/news/prime-insights/2018-insights/insights-RI3_HAEcase.html
Related news
Perspectives
April 25, 2024
Drug Approvals Monthly Update: April 2024
This monthly update of United States (U.S.) Food and Drug Administration (FDA) approvals…
Perspectives
April 24, 2024
Prime/MRx resident wins AMCP Foundation Best Poster Award
Ai Quynh Nguyen, PharmD, was recently recognized for her research on opioid-prescribing patterns and outcomes
Perspectives
April 23, 2024
Expert Clinical Network Insights: April 2024
A look into our Expert Clinical Network (ECN) – part of Prime/MRx’s value-based approach to medical and pharmacy benefit management that offers access to more than 175 national and world-renowned key opinion leaders in multiple disease categories who provide expertise on challenging prior authorization case reviews, peer-to-peer discussions, drug policy development and formulary guidance