Perspectives
Understanding specialty drug costs and how to manage them
A look at the specialty landscape and how Prime delivers value to employers
May 22, 2023Many employers are seeing increases in drug spend, often driven by high-cost medications called specialty drugs, which are used to treat several severe diseases and conditions.
With the increase in costly treatments and the growing prevalence of high-cost diseases, employers simply can’t afford to wait and see. A specialty strategy has become an essential element of a successful benefits program.
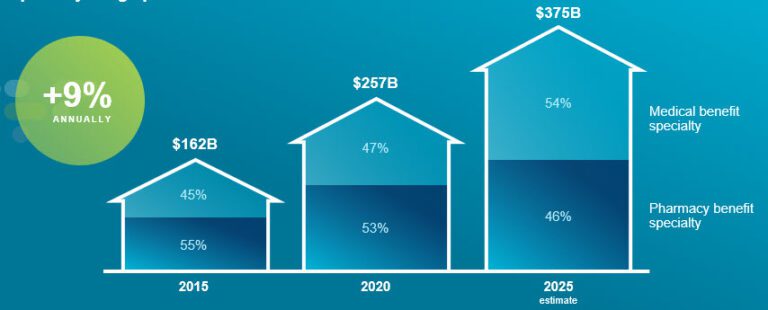
Specialty drug spend began increasing in a big way in the mid-2010s. In 2015, it totaled $162 billion. By 2025, it’s estimated that specialty drug spend will reach $375 billion.1
Total specialty drug spend1
Additionally, a full half of specialty drug spend passes through the medical benefit. This makes it essential that policies are coordinated across both the medical and pharmacy benefit for both cost management and patient care.
Why it matters to employers: Many people living with specialty diseases still work
Specialty medications can also be significantly more expensive than traditional prescriptions. And many people living with specialty diseases are still working, which can drive up health care costs significantly for employers. In fact, just 2% of employees account for 50% of all drug spend. In addition, high-cost individuals are 33% more likely to stay on their plans.2,3
A small group of employees can have a significant impact on employer spend4
Specialty drugs have seen substantial growth
And key specialty drugs have seen substantial growth. For instance, specialty drugs used to support autoimmune conditions and oncology now total 68% of total specialty drug spend.4
Why it matters to employers: Employees face rising costs and pressures
As drug therapy costs rise, employees’ out-of-pocket costs also go up. Complex conditions create pressure on the entire family. That can impact a range of social determinants of health, like economic stability, support systems and transportation. As more of these therapies come to market, employers can focus on improving affordability and remove barriers to a positive patient experience, while also helping them manage the tremendous cost challenges these new therapies bring.
For instance, many people using specialty drugs require sophisticated management with support from experts that are matched by condition. What’s more, 80% of patients taking a specialty drug have at least one other condition.
How does Blue and Prime deliver a solution?
Now more than ever, employers need value-driven solutions and transparent delivery models. And integrated solutions and strategies – across both medical and pharmacy benefits – can help employers navigate the complicated and evolving specialty landscape.
- With our acquisition of Magellan Rx, Prime Therapeutics (Prime) offers industry-leading specialty expertise and flexible solutions to help employers improve care, stay ahead of trend and reduce specialty spend across both pharmacy and medical benefits.
- Our deep understanding of pharmacy trends and future-focused strategies for emerging therapies and spend categories underscores our market-leading position and commitment to cost-effective and high-quality care.
- Working with your Blue Plan, we tap into insights and analytics to improve the health care experience from beginning to end.
- Our best-in-class teams develop comprehensive solutions to tackle some of the highest-cost and most challenging disease states (e.g., oncology, diabetes, hemophilia, etc.) and complex therapies.
- And we back this with guaranteed outcomes because we have the data and expertise to manage drug therapy opportunities across an integrated ecosystem, providing a full view of clinical and financial factors pertaining to drug and medical benefits.
As we build for the future, we envision a specialty care model that improves the experience for members from prescription intake to fulfillment while eliminating complexities, driving savings and reducing waste.
With Blue and Prime, employers and their employees benefit from holistic care that closes the gaps between medical and pharmacy benefits.

State of specialty
Understanding the specialty landscape
Specialty drugs have changed pharmacy over the past decade and now represent more than half of total drug spend. And having a strong specialty strategy that spans pharmacy and medical benefits has never been more essential to the success of your business.
References
- Values are net of rebates. Source: Nephron Research, Evaluate Pharma
- Jackson EA, et al. JMCP 2021;27(6):753-759. (2021). An analysis of member retention patterns for adult rare disease cohorts to support evaluating multiyear payment arrangements for novel therapies. https://www.jmcp.org/doi/pdf/10.18553/jmcp.2021.27.6.75
- Fang H, Frean M, Sylwestrzak G, Ukert B. Trends in Disenrollment and Reenrollment Within US Commercial Health Insurance Plans, 2006-2018. JAMA Netw Open. 2022;5(2):e220320. Published Feb 1, 2022. doi:10.1001/jamanetworkopen.2022.0320
- Prime Book of Business, 2023
- IQVIA Institute for Human Data Science. (2022, April). The use of medicines in the U.S. 2022. https://www.iqvia.com/-/media/iqvia/pdfs/institute-reports/the-use-of-medicines-in-the-us-2022/iqvia-institute-the-use-of-medicines-in-the-us-2022.pdf
Related news
Perspectives
July 25, 2024
Quarterly Drug Pipeline: July 2024
Clinical insights and competitive intelligence on anticipated drugs in development
Perspectives
July 22, 2024
Oncology Insights: 2024 ASCO Annual Meeting key findings
Findings from this year’s American Society of Clinical Oncology (ASCO) Annual Meeting will likely lead to clinical practice changes and U.S. Food and Drug Administration (FDA) drug approvals or expansions
Perspectives
July 16, 2024
LISTEN NOW: Beyond the business – Stories of corporate kindness | Pharmacy Friends Podcast
In this episode, we talk about how our employees' help goes beyond our work in health care, aiding in philanthropic efforts