Perspectives
Reducing opioid use among outliers; are we doing enough?
Prime helps health plans address members whose opioid use puts them outside the norm
June 15, 2018Prime has achieved a 79 percent decline in high-risk opioid outliers over five years.¹ But the outlier population is small, and the opioid epidemic is huge. It killed 52,000 last year, more people than car crashes, HIV/AIDS, gun deaths and gun homicides.²
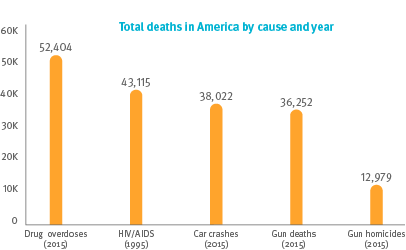
Is the reduction in the outlier population good?³ Yes. Is it enough? No. Can we do more? Yes.
Who is an outlier and why are we concerned with them?
The purchasing behaviors of outliers are different than the rest of a particular group or data set. They are outside the norm. They tell us there might be something wrong.
For most needs, members get a short (3-day) prescription of a short-acting, low-dose opioid. They pick it up from their usual pharmacy. Chronic pain and cancer pain guidelines are different. But outliers fall even outside of those.
An outlier has an average daily morphine milligram equivalent (MME) of 90mg or higher. They receive opioids from more than three prescribers and more than three pharmacies. Or they might get their opioids from more than five prescribers regardless of number of pharmacies over a six-month period.
How did the outlier group change and why?
In the first half of 2012, 1,255 members (12 per 100,000) were identified as high-risk outliers. Five years later, in the second half of 2017, outliers were reduced to 351 members (2 per 100,000). Prime’s Controlled Substance Management Program, in concert with its health plan clients’ efforts, contributed to this reduction.1
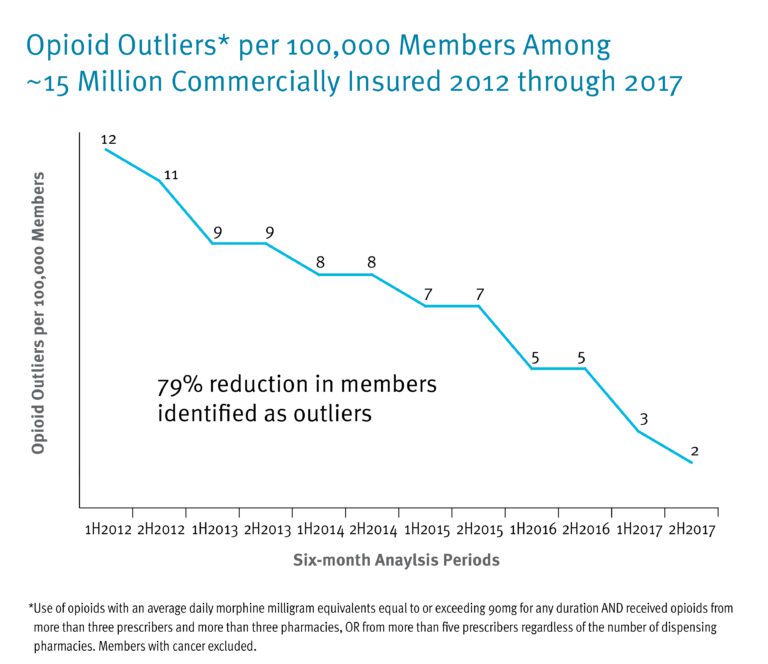
Prime also found a 16 percent reduction in tablet and capsule opioid claims per capita from January 2012 through June 2017. Other opioid utilization metrics that decreased over the past five years include the percent of members with an opioid claim (decreased 8.1 percent) and quantity dispensed divided by days supply (decreased 9.1 percent).³
Can we do more?
Yes. From a business perspective, substance use and abuse is expensive. Many employees with substance abuse issues may not yet show up in medical or pharmacy claims. And there are the nonmedical costs to your business.
The National Safety Council (NSC) estimates that substance use costs $1.7 million annually in lost time, job turnover, retraining and health care for a service business with 5,000 employees in the Midwest. The NSC give plan sponsors an estimate of costs by industry, geography and size. They provide employer materials on drug testing, workers’ compensation, prevention and more.
What is Prime doing?
Prime is seeing very positive outcomes from our data and analysis of opioid claims. We will continue to do more. We need to continue improving. For example, we will encourage adoption of days’ supply and quantity limits for new opioid prescriptions in accordance with the Center for Disease Control and Prevention’s (CDC) guidelines.
Prime is an active contributor to the national conversation on opioid management. Last fall, my colleague, Patrick Gleason, Prime’s senior director, health outcomes, contributed to a cross-functional opioid epidemic report that includes and proven recommendations for how private and public organizations can help prevent misuse and non-medical use of opioids and all controlled substances.
We will continue developing and improving our clinical programs that address opioid misuse and abuse. All stakeholders need to keep the momentum strong so we can build upon the progress we’ve made.
References
- Poster: “Opioid utilization and cost – a 5 year look among 15 million commercially insured members. Starner, CI; Gunderson, BW, Gleason, PP. September , 2017. Presented at Fall AMCP October 2017 Orlando, FL. https://www.primetherapeutics.com/content/dam/corporate/Documents/Newsroom/Pressreleases/2017/documents-amcpposter2017-opioids.pdf. News release: https://www.primetherapeutics.com/en/news/pressreleases/2017/amcp-opioid-release.html
- Opioid statistic and chart How the opioid epidemic became America’s worst drug crisis ever, in 15 maps and charts.” By German Lopez and Sarah Frostenson. Mar 29, 2017. Vox Media. Vox Media, Inc.© https://www.vox.com/science-and-health/2017/3/23/14987892/opioid-heroin-epidemic-charts
- Prime launches comprehensive program to address opioid and controlled substance abuse. July 17, 2017. Accessed at: https://www.primetherapeutics.com/en/news/pressreleases/2017/opioid-epidemic-release.html
Related news
Perspectives
July 25, 2024
Quarterly Drug Pipeline: July 2024
Clinical insights and competitive intelligence on anticipated drugs in development
Perspectives
July 22, 2024
Oncology Insights: 2024 ASCO Annual Meeting key findings
Findings from this year’s American Society of Clinical Oncology (ASCO) Annual Meeting will likely lead to clinical practice changes and U.S. Food and Drug Administration (FDA) drug approvals or expansions
Perspectives
July 16, 2024
LISTEN NOW: Beyond the business – Stories of corporate kindness | Pharmacy Friends Podcast
In this episode, we talk about how our employees' help goes beyond our work in health care, aiding in philanthropic efforts