Perspectives
Managing drug costs for ultra-rare genetic conditions
The implications of funding big buck gene therapy treatments
April 27, 2020Together, these rare conditions total up to a significant population
In the United States, a rare disease is defined as a condition that affects fewer than 200,000 Americans (or about 620 people per million). Though definitions vary, an ultra-rare disease can be thought of as one that affects fewer than 20 Americans per million (or one person per 50,000.)1-3
Clinical innovation has brought about curative treatments for rare, genetic conditions. These new treatments are a welcome relief for patients. But they come at a steep cost to payers. With current costs at more than $2 million for a single treatment, even one member with a claim for a gene therapy treatment could be financially devastating for a payer.
Prime’s experts proactively monitor and analyze the drug pipeline and follow critical market trends. This in-depth understanding and market alignment drive ongoing innovation and new approaches for specialty solutions. The latest innovation is a financial product specifically designed to reduce the financial risks that go along with high-cost gene therapy.
This one-of-a-kind financial product would not have been possible without:
- Market-leading research into the cost of care
- A strong portfolio of value-based contracts
- Extensive alignment with health plans
- Expert health outcomes researchers
- Experience in managing medical and pharmacy benefit claims
These are all elements Prime brings to the challenge.
Financial protection for plan sponsors
PreserveRx is a new reinsurance product providing an extra layer of high cost gene therapy financial protection. Unlike traditional reinsurance products that have coverage starting at a much higher threshold, frequently at a million dollars or more, this protection kicks in at a minimum $250,000 threshold.
Plans purchasing traditional reinsurance products often only reach the higher threshold when expensive medical services like extended hospital stays and surgeries are billed. PreserveRx protects payers when the covered gene therapies causes them to meet the lower threshold.
Prime partners with BCS Insurance Company (BCS) to offer this coverage. Both Prime and BCS have longstanding relationships with Blue Plans. BCS serves Blue Cross and Blue Shield companies and commercial markets across America and is owned by all primary Blue Cross and Blue Shield licensees.
The PreserveRx offering has two parts:
- The financial component, from BCS, seeks to provides payer relief associated with one of the covered gene therapies.
- Its clinical services component, from Prime, leverages integrated medical and pharmacy claims data, clinical research and expert analysis to forecast financial impact and potential use for these rare conditions. Medical policy criteria help ensure that the right patient receives the right treatment.
- PreserveRx provides access to savings created through outcomes-based contracts that track and report outcomes over many years to help ensure the therapy works as claimed.
Prime’s experience helps make this happen
Prime’s research to identify the number of drug super spenders – members with pharmacy and medical drug therapy claims totaling $250,000 or more annually – provided the foundational insights that guided the development of PreserveRx.9
The initial offering of PreserveRx will cover the following drugs
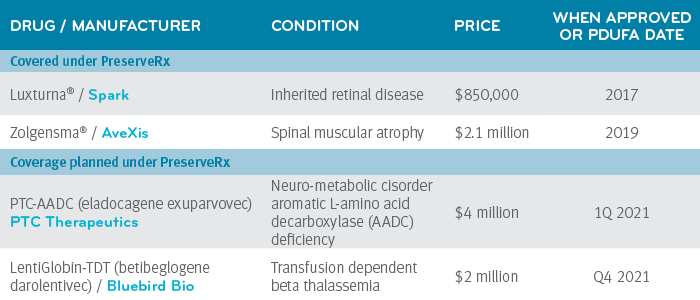
Plans also have the option to only cover the two currently FDA-approved gene therapies: Zolgensma and Luxturna.
This is just one innovation; many more will be needed
Treating just 5 percent of the people with rare and ultra-rare diseases at $850,000 a year would cost nearly $1.3 trillion. That’s four times what the United States spends on all prescription drugs today ($330 billion).10
Each drug and each condition require its own strategic approach with its own analytics. Above all, a plan must coordinate strategy across both the medical and pharmacy benefits. Prime’s strategy for managing medical drug spend has evolved over two decades of working with our clients’ medical benefit data. Experience in the nuances and limitations of medical data gives us an advantage. We know how to interpret and apply data to create customer-centric knowledge.
This helps us keep the patient at the center of the decision-making process.
When it comes to the drugs that treat rare and ultra rare conditions, all of Prime’s drug management tools come into play. Understanding how to apply those tools across both the pharmacy and medical benefits becomes even more important when drug prices get bigger.
The ultra-high drug pricing we see today is unsustainable.11,12,13 A lot of things have to change. There’s a lot of work ahead of us. But we’re confident PreserveRx is a good step in the right direction.
References
- Harari S. Why we should care about ultra-rare disease? Eur Respir Rev 2016; 25: 101–103.
- Orphan Drugs in the United States: Growth Trends in Rare Disease Treatments, Oct 17, 2018. IQVIA Institute Report. Accesed at: https://www.iqvia.com/-/media/iqvia/pdfs/institute-reports/orphan-drugs-in-the-united-states-growth-trends-in-rare-disease-treatments.pdf
- FAQs About Rare Diseases, U.S. Department of Health & Human Services, National Institutes of Health. Genetic and Rare Diseases Information Center (GARD). Accessed at: https://rarediseases.info.nih.gov/diseases/pages/31/faqs-about-rare-diseases
- U.S. Food and Drug Administration. Press release. “FDA approves novel gene therapy to treat patients with a rare form of inherited vision loss.” December 18, 2017.
- SMA Foundation. https://www.togetherinsma.com/en_us/home/introduction-to-sma/smn1-gene.html
- National Hemophilia Foundation. https://www.hemophilia.org/
- Centers for Disease Control. “Thalassemia Awareness.” https://www.cdc.gov/features/international-thalassemia/index.html. Accessed on January 9, 2020.
- National Institutes of Health. National Library of Medicine. Genetics Home Reference. https://ghr.nlm.nih.gov/condition/aromatic-l-amino-acid-decarboxylase-deficiency. Accessed on January 9, 2020.
- Bowen K, Gleason P. Drug Super Spenders:2016-2018 Growth in Number of Members and Total Pharmacy Plus Medical Benefit Drug Cost for Members with Extremely High Annual Drug Cost in a 17 Million Member Commercially Insured Population. Academy of Managed Care Pharmacy: National Harbor, MD. J Manag Care Spec Pharm 2019:25(10-a):S90. https://www.jmcp.org/doi/pdf/10.18553/jmcp.2019.25.10-a.s1
- Prescription Drug Spending in the U.S. Health Care System, March 2018. ©2020 American Academy of Actuaries Accessed at: https://www.actuary.org/content/prescription-drug-spending-us-health-care-system
- Modifications to the ICER value assessment framework for treatments for ultra?rare diseases, Final Version, November 2017. Accessed at: https://icer-review.org/wp-content/uploads/2017/11/ICER-Adaptations-of-Value-Framework-for-Rare-Diseases.pdf
- “ICER draws new gene therapy pricing framework,” by Jonathan Gardner. HealthCareDive. Nov. 13, 2019. Accessed at: https://www.healthcaredive.com/news/icer-gene-therapy-one-time-pricing-framework/567253/
- Starner CI, Gleason PP. Spinal Muscular Atrophy Therapies: ICER Grounds the Price to Value Conversation in Facts. Journal of Managed Care and Specialty Pharmacy 2019:25(12):1306-1308. https://www.jmcp.org/doi/abs/10.18553/jmcp.2019.25.12.1306
Related news
Perspectives
July 25, 2024
Quarterly Drug Pipeline: July 2024
Clinical insights and competitive intelligence on anticipated drugs in development
Perspectives
July 22, 2024
Oncology Insights: 2024 ASCO Annual Meeting key findings
Findings from this year’s American Society of Clinical Oncology (ASCO) Annual Meeting will likely lead to clinical practice changes and U.S. Food and Drug Administration (FDA) drug approvals or expansions
Perspectives
July 16, 2024
LISTEN NOW: Beyond the business – Stories of corporate kindness | Pharmacy Friends Podcast
In this episode, we talk about how our employees' help goes beyond our work in health care, aiding in philanthropic efforts